Orthopedics: The term was coined by Nicolas Andry. Ortho means straight and pedics means child so orthopedics means Straight child.
Definition of orthopedics: The branch of surgery that deals with the prevention or correction of injuries or disorders of the skeletal system and associated muscles, joints and ligaments.
- Father of Orthopedics—Nicolas Andry.
- Father of Modern Orthopedics—Robert Jones.
- Father of Arthroplasty—John Charnley.
- Father of Arthroscopy—Kenji Takagi and Masaki Watanabe
- Father of orthopedic oncology—Enneking
- Plaster of Paris (CaSO4 ½ H2O): Mathysen
ROLE OF IMAGING IN ORTHOPEDICS
X-rays are usually the first radiological investigation done in orthopedics and its uses involves screening of Cortex and Marrow. X-rays are the first investigations in traumatic disorders.
Soft tissue planes (muscle and fat planes) are visualized on X-rays and often students forget this!
(Loss of soft tissue planes is earliest X-ray changes in infection/swelling in limb and it is seen after 24–48 hours of onset of disease they are more useful for infections than tumors).
- Glass pieces are visualized on X-rays due to presence of lead in them.
- Cartilage is not seen on X-ray.
Ossified tissue (Live bone) is like a brick wall! (Fig. 1.3A) | Calcified tissue/dead bone is like a chalk! (Fig. 1.3A) |
|---|---|
Properly laid down Architecture of haversian and volkmann's Canal with calcified hydroxyapaetite crystals. | Deposition of calcium salts without bony architecture/trabeculae. |
Live bone looks less white on X-rays and is strong in strength. | Dead bone looks more white on X-rays as compared to surrounding normal bone. |
Live bone (e.g. Brick wall) is stronger, heavier but less white on X-rays (osteopenia or rarefaction) and dead bone (e.g. chalk) is light and white (Sclerosed on X-ray) (Figs. 1.3A to C).
Periosteum has two layers outer Fibrous layer (non-functional layer) and inner Cambium layer (Cellular layer/active layer). It does not contain dense regular connective tissue as seen in tendon, ligament and aponeurosis. Roles of cambium layer are:
- Bone union: Cambium layer has important role in bone union at fracture site by providing the osteoprogenitor cells. If cambium layer is deficient bone union is difficult, e.g. neck of femur cambium layer is universally absent hence this is one of the causes of higher rates of non-union in femoral neck fractures.
- Origin of bone tumors: Since cambium layer is cellular layer it is more prone to give origin to bone tumors, e.g. osteochondroma. Treatment principle of any bone tumor is to remove the tumor along with cells of origin so in such tumors surgical management consists of tumor excision along with periosteum and failure to remove the periosteum would cause recurrence of the tumor.
- Periosteal reaction: Whenever a disease pathology destroys the bone cambium layer is irritated and responds by periosteal reaction, that is bone formation under the periosteum. Thus periosteal reaction is an indicator that disease is destroying the bone.
Types of Periosteal Reaction
- No reaction: Tuberculosis of bones do not usually have a periosteal reaction.
- Narrow zone of activity, e.g. Solid periosteal reaction (single layer of periosteal elevation) is seen in benign lesion like, Benign tumors or Pyogenic Osteomyelitis.
- In case of osteomyelitis the periosteal reaction is seen on day 7 to 10th (or 2nd week or day 10th).
In malignant lesions there is wide area of activity, e.g. Onion peel/codman's triangle and sunray appearance (all are indicative of wide area of activity).
Onion peel or lamellated appearance—Seen in any malignant or chronic lesions (e.g. chronic osteomyelitis) but usually ewing's sarcoma.
Codman Triangle—Triangular bony growth seen at angle of lifting of periosteum, it can be seen in any malignant lesion but usually osteosarcoma.
Sunray appearance/sunburst/spiculated appearance – Calcification along the Sharpey's fibres, can be seen in any malignant lesion but usually osteosarcoma.3
Osteophytes—(Osteo means bone and phytes means growth) They are seen in case of joint damage.
Syndesmophytes indicates Spine destruction (Osteophyte of spine) but they bridge across the joint as compared to osteophytes which are non-bridging.
Ultrasound (USG): Now-a-days there is increasing role of USG in assessment of various joint and soft tissue pathologies.
- High frequency transducers are used (5–12 MHz).
- It provides the benefit of real-time imaging and evaluation of soft tissue near a metallic orthopedic hardware without the artifact that limits MR imaging.
- USG is specially useful in evaluation of muscles and tendons.
- Due to subjective variations in ultrasound results, MRI has replaced its use for many indications.
CT Scan: CT Scan is the investigation for cortex and calcification.
Any new bone formation or 3D image—CT Scan is preferred investigation.
MRI is investigation of choice for Marrow, Soft tissues (Brain/Spinal cord/Ligaments/Tendons/nerves/vessels) and Cartilage.
Basic Images in MRI are T1 and T2
- T1 – 1st professional subject anatomy—so in T1 image anatomy is seen.
- T2 – 2nd professional subject pathology—so in T2 image Pathology is seen.
‘Water is white on T2’
Water is any body fluid example, synovial fluid/C.S.F/inflammatory or traumatic edema.
Please Note:
Any occult fracture (not visualised on X-ray) e.g. Fracture neck femur ~ MRI is investigation of choice.
Any fracture in which there is marrow edema example stress fracture – MRI is investigation of choice.
Osteomyelitis starts in marrow of metaphysis—MRI is best radiological investigation.
Tumors with marrow involvement, any micrometastasis or soft tissue component—MRI can aid in diagnosis.
Avascular Necrosis/Perthes disease (avascular necrosis of femoral epiphysis)-MRI is investigation of choice.
Note: CT scan can principally show only the bony structures whereas MRI can show the soft tissues very well.
Figs 1.14A and B: (A) CT Scan mainly shows the bony structure whereas (B) MRI Shows Bone, Soft tissues and cartilage
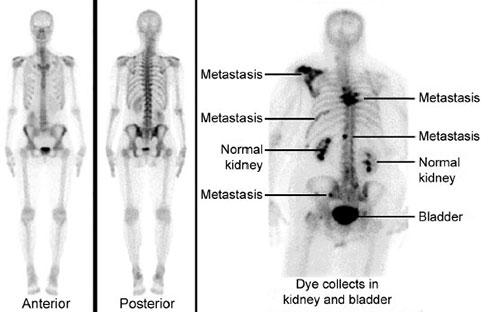
TC labelled bone scan: Can pickup—Blastic (Osteoblastic) activity—methylene diphosphonate is taken up by osteoblasts on scanning the whole skeleton.
Bone scan show activity in areas with increased osteoblastic activity example tumors, infection or fracture. Thus in cases with bilateral stress fractures bone scan is preferred investigation.
It can pick up tumors that go from one bone to other, i.e. bone to bone metastasis.
BONE: Bone to bone/Osteosarcoma/Neuroblastoma/Ewing sarcoma (maximum incidence)
Limitation: Bone Scan cannot identify the source of unknown primary.
PET CT: Position emission tomography + CT Scan for whole body. It is a combination of 2 modalities.
18 F Deoxy glucose uptake by tumor cells (as they have anaerobic metabolism) and CT scan for all viscera so it can identify unknown primary. (Bone Scan the uptake is by osteoblast and PET Scan by tumor cells)
Thus PET–CT is more useful than Bone Scan as it can identify primary and is more specific for tumor cells.
Limitation: Osteoblastic lesions have limited uptake on PET so bone scan may be more valuable.
Metastasis |
|---|
|
Remember that radiological diagnosis in cases of infection and tumors is suggestive never diagnostic.
Diagnostic is always tissue diagnosis
Tumors and infection can mimic each other (clinically and radiologically), e.g. Osteosarcoma and Ewings sarcoma are two tumors that mimic osteomyelitis. (Both have accompanying fever and increased local temperature).
Tumors and bone infections are usually metaphyseal and both need tissue diagnosis for differentiation.
- Thus, Culture is gold standard for infection
- So rule is Culture all biopsies, biopsy all cultures. That is whenever you obtain any sample from a suspected case of tumor or infection divide it into two parts send one for culture and other for histopathology.
Osteomyelitis
- Pyogenic Osteomyelitis on X-rays will show loss of soft tissue planes after 24–48 hours (1st change).
- Day 7 to 10-solid periosteal reaction is identified. (1st Bony change)
- In tuberculosis there is no periosteal reaction.
- Chronic osteomyelitis—sclerosed dead bone (sequestrum) is important for diagnosis and onion peel appearance is the usual periosteal reaction.
- MRI can pick up marrow changes in metaphysis. (Best radiological investigation for Osteomyelitis and Tuberculosis).
- Bone scan is next in preference to MRI to pick up infections by picking osteoblastic activity at the site of infection.
- Culture and growth of organism is most definitive diagnostic modality for Osteomyelitis.
Bone Tumors
- X-ray is to localize the tumor.
- CT scan is for extent and cortical lesion.
- MRI is for Marrow extent, micrometastasis and soft tissue involvement (Most preferred investigation for most tumors).
- PET-CT and Bone scan for multiple lesions (PET-CT is better than Bone Scan).
- Biopsy is definitive diagnostic modality for any tumor.
MRI in Developmental Dysplasia of Hip (DDH)
- T1W images display exact position of the cartilage which is useful when position of the same is uncertain on X-rays or serial follow up is required, thereby reducing radiation exposure.
- Useful in patients with or without plaster casts.
- When ossific nucleus is not visible on plain X-ray or CT.
- T2W images are useful for complications like ischemic necrosis and effusions which are not demonstrated with USG or X-ray.
- 3D MR rendering for complex femoral head and acetabular special relationships and dysplasias.
USG in DDH
- Evaluation of cartilaginous femoral head prior to appearance of ossific nucleus, subluxation, dislocation, pulvinar or inverted labrum, hypoplastic ossific nucleus, acetabular dysplasia and ossification. The findings in USG are subjective and are not as specific as MRI.
Thus if the question is asked for screening of neonatal hip or hip instability then USG is investigation of choice.
If the question is asked about Investigation of choice for DDH than MRI >USG will be the order as MRI will be more useful for assessment of complete disease spectrum, management and complications of DDH.
MULTIPLE CHOICE QUESTIONS
1. Stress fractures are diagnosed by: (JIPMER May 2016, AIIMS May 2015, AI 2004)
- X-ray
- CT
- MRI
- Bone scan
Ans. is ‘C’ MRI (Investigation of choice for unilateral stress fracture is MRI and for bilateral is Bone Scan), when it is not mentioned unilateral or bilateral, MRI is preferred answer.
2. Image of knee joint, which investigation is being done? (AI 2016)
- MRI Coronal section
- MRI Sagittal section
- CT Coronal section
- CT Sagittal section
Ans. is ‘B‘ MRI Sagittal section
3. Acute Osteomyelitis, earliest bone change can be best seen by? (AI 2016)
- PET CT
- MRI
- Bone Scan
- X-ray
Ans. is ‘B’ MRI > ‘C’ Bone Scan
4. Identify the marked structure: (AI 2016)
- Trapezium
- Lunate
- Trapezoid
- Capitate
Ans. is ‘B’ Lunate
5. Which of the following is the investigation of choice for Perthes disease of the bone? (JIPMER 2015)
- MRI
- CT
- X-ray
- USG
6. Sunray appearance on X-ray is seen in (NEET 2015)
- Osteosarcoma
- Osteochondroma
- Osteoclastoma
- Chondroblastoma
Ans. is ‘A’ Osteosarcoma
7. Occult fracture of neck femur is best diagnosed by (PGM-CET 2015)
- CT Scan
- Bone scan
- MRI
- None of the above
Ans. is ‘C’ MRI
8. Sunray appearance in osteosarcoma is due to: (AIIMS Nov 2014)
- Periosteal reaction
- Muscle fibre calcification
- Blood vessel calcification
- Bone resorption
Ans. is ‘A’ Periosteal reaction
9. A child with injury in hand with glass pieces next investigation would be: (AIIMS Nov 2014)
- X-ray
- USG
- MRI
- CT Scan
Ans. is ‘A’ X-ray
10. Dense regular connective tissue fibres are seen in all except: (AIIMS Nov 2014)
- Periosteum
- Tendon
- Ligament
- Aponeurosis
Ans. is ‘A’ Periosteum
11. Developmental Dysplasia of Hip (DDH) best diagnostic modality is: (Neet Pattern 2014, May AIIMS 2012)
- Clinical
- X-ray
- MRI
- CT
Ans. is ‘C’ MRI
12. A 4-year-old girl with fever and mass in thigh, on her X-ray there is periosteal reaction and destruction of bone. Next investigation to be done in this girl is: (AIIMS Nov 2013)
- Bone biopsy
- Bone scan
- Blood culture
- CT Scan
Ans. is ‘A’ Bone biopsy
(Order is X-ray → MRI → Bone biopsy)
13. A 10-year-old obese child from endocrinology department was referred to emergency for a painful limp with hip pain which of the following investigation is not required: (AIIMS Nov 2013)
- X-ray of the hip
- MRI of the hip
- CT scan of hip
- USG of hip
Ans. is ‘C’ CT scan of hip
This is a Obese Limping child with hip pain the possible differential diagnosis will be
Osteomyelitis (X-MAS)
Septic arthritis (X-MAS)
Slipped capital femoral epiphysis (X-MRI)
Transient synovitis (X-MAS)
Hence CT will be least preferred. Previously CT Scan was carried out for SCFE but now MRI has replaced its indication.
14. 4-year-old child complains of pain and swelling of right tibia on evaluation patient has high ESR, leucocytosis and on X-ray tibial lesion best investigation is: (AIIMS Nov 2012)
- Blood C/S
- Pus C/S
- MRI
- Biopsy
Ans. is ‘D’ Biopsy
15. Periosteal reactions is seen in: (NEET Pattern 2012)
- Osteomyelitis
- Syphilis
- Tumor
- All
Ans. is ‘D’ All
16. Screening of neonatal hip instability most commonly used modality is: (NEET Pattern 2012)
- USG
- X-ray
- MRI
- CT
Ans. is ‘A’ USG
17. Bilateral stress fractures are diagnosed by: (NEET Pattern 2012)
- X-ray
- CT
- MRI
- Bone scan
Ans. is ‘D’ Bone Scan
18. 45-year-old female has history of slip in bathroom complaints of pain right hip, tenderness in scarpas triangle and normal X-ray. Next investigation is: (May AIIMS 2012)
- USG guided aspiration
- CT
- MRI
- Bone scan
Ans. is ‘C’ MRI
This case refers to post-traumatic pain in proximal femur, scarpas triangle refers to area of femoral neck and for stress or occult fracture of neck femur where traumatic marrow edema is seen – MRI is investigation of choice.
19. Tuberculosis of spine best diagnostic modality is: (May AIIMS 2012)
- Clinical
- X-ray
- MRI
- CT guided biopsy
Ans. is ‘D’ CT guided biopsy
Tissue diagnosis is always preferred over any radiological diagnosis hence CT guided biopsy to obtain tissue and than further investigations to grow the organisms is the preferred approach. Many make a mistake of marking MRI as the answer please remember that MRI is best radiological investigation but best investigation overall for infections or tumors is always biopsy.
20. Multiple Bone metastasis are diagnosed by: (AI 2011/AIIMS Nov 2010)
- X-ray
- CT
- MRI
- Bone scan
Ans. is ‘D’ Bone Scan
21. Best investigations for multiple bone metastasis: (NEET Pattern 2012)
- PET CT
- CT
- MRI
- Bone scan
Ans. is ‘A’ PET CT
For bone metastasis PET CT is better than bone scan.
22. What is the earliest change of osteomyelitis on X-rays: (AIIMS May 2010)
- Loss of soft tissue planes
- Periosteal reaction
- Sequestrum
- Lytic defects
Ans. is ‘A’ Loss of soft tissue planes
23. What is the earliest bony change of osteomyelitis on X-rays? (AIIMS Nov 2009)
- Loss of soft tissue planes
- Periosteal reaction
- Sequestrum
- Lytic defects
Ans. is ‘B’ Periosteal reaction
Pyogenic osteomyelitis on X-ray in 24–48 hours will show loss of soft tissue planes (earliest change on X-ray).
Day 7 to 10-solid periosteal reaction (earliest bony change on X-ray).